Causes of Pelvic Folliculitis
Folliculitis is a common skin condition where hair follicles become inflamed. It’s not unusual to find it occurring in the pelvic area, among other regions of the body. This condition can be both uncomfortable and frustrating, but understanding why it happens can help you manage it effectively.
Here, we will take a closer look at the causes of pelvic folliculitis, how you might identify it, and what steps you can take to soothe the affected area.

What Is Folliculitis?
Essentially, it’s the inflammation of one or more hair follicles, which can appear anywhere on your skin, including the pelvic area. This inflammation often results in red, bumpy, sometimes pus-filled pimples around hair follicles. These bumps can be itchy, tender, and even painful.1
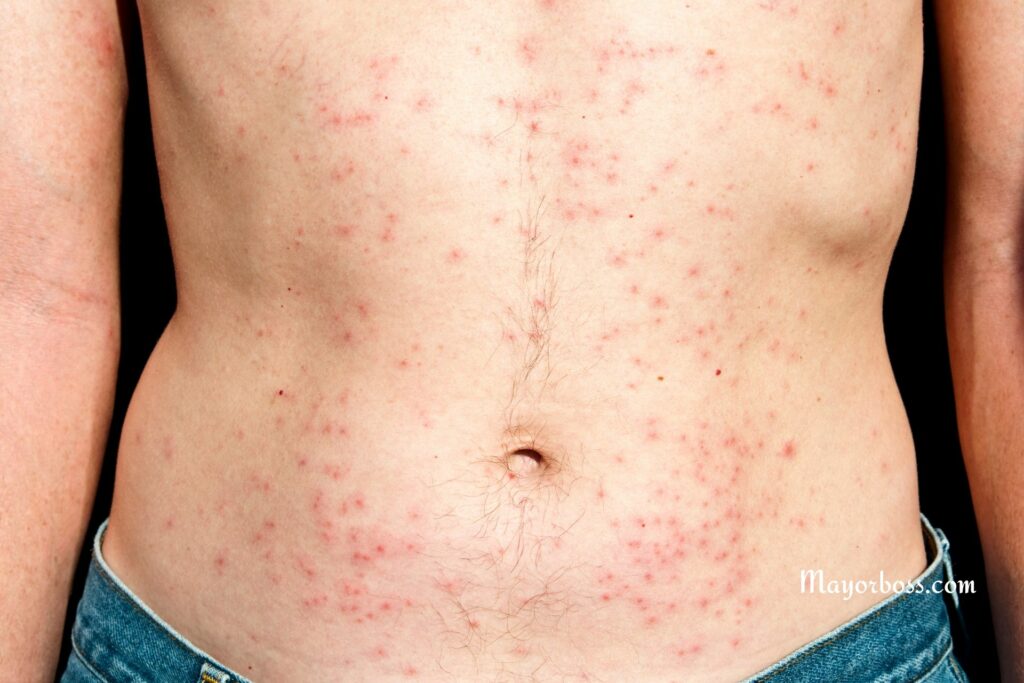
Main Causes of Pelvic Folliculitis
Several factors can contribute to the development of pelvic folliculitis. Here are the most common culprits:
Bacterial Infection
The most frequent cause of folliculitis is an infection with Staphylococcus aureus (staph) bacteria. Your skin naturally harbors these bacteria, but they can cause problems if they enter your body through cuts or other wounds.2
Fungal Infections
In some cases, a fungus rather than bacteria can infect hair follicles. This is less common but can occur in the pelvic area, especially if the environment is warm and moist, creating an ideal setting for fungi to thrive.
Irritation from Shaving or Waxing
Shaving or waxing the bikini area can irritate the skin and hair follicles, leading to inflammation. This type of folliculitis is often referred to as “razor bumps” or “hot tub folliculitis” if caused by a spa’s poorly chlorinated water.3
Friction from Clothing
Tight clothing can cause friction and sweating in the pelvic area, which may irritate and inflame hair follicles. Synthetic fabrics that don’t breathe well increase the risk.
Blocked Follicles
Oil, sweat, and dead skin cells can block hair follicles, leading to folliculitis. This is why it’s essential to maintain good hygiene, particularly in areas prone to sweating.
Identifying Pelvic Folliculitis
You can usually recognize pelvic folliculitis by the appearance of red, inflamed bumps around hair follicles. These may be itchy or painful and could have pus. If you’re experiencing these symptoms, it’s a good idea to consult a healthcare provider for an accurate diagnosis and appropriate treatment.
Managing and Preventing Pelvic Folliculitis
Thankfully, there are steps you can take to manage and prevent pelvic folliculitis:
- Maintain Good Hygiene: Regular washing with a gentle cleanser can help remove bacteria and debris that could lead to folliculitis.
- Use Proper Shaving Techniques: If you shave, use a sharp razor, shave in the direction of hair growth, and apply a soothing moisturizer afterward.
- Wear Breathable Clothing: Choose loose-fitting clothes made from natural fibers to reduce friction and allow your skin to breathe.
- Avoid Sharing Personal Items: Towels and razors can harbor bacteria, so it’s best to keep these items to yourself.
If you follow these guidelines and still find yourself dealing with persistent folliculitis, a healthcare provider can offer treatments like topical creams, oral antibiotics, or other medications to help clear the infection and reduce inflammation.
Frequently Asked Questions
- Can pelvic folliculitis spread to other areas? Yes, if caused by an infectious agent like bacteria or fungi, it can spread to adjacent skin areas if not properly treated.
- Is folliculitis sexually transmitted? No, folliculitis itself is not sexually transmitted. However, bacteria or fungi causing the condition can be spread through close physical contact.
- How long does pelvic folliculitis last? With proper treatment, symptoms of folliculitis usually improve within a few days. However, it can become a recurring issue if the underlying cause isn’t addressed.






